
NO Subsidy
Health Insurance
Purchase Health Insurance
With NO Subsidy
OFF Exchange
You have been directed to this page because…
You Make Too Much Money


Or
You Do Not Want a Subsidy


Why No Subsidy?
If you do not want a subsidy, or make too much money to qualify for a subsidy, you can shop for health insurance OFF Exchange (in the private market). In Nevada we have HMO, EPO, and PPO health insurance plan options available to enroll into. When you buy a health insurance plan in the private market, you don’t need to disclose your income or worry about updating your account throughout the year. You set it and forget it. In addition, the prices “OFF Exchange” are often less expensive than “ON Exchange”.
These plans are Qualified Health Plans that contain the 10 Essential Health Benefits that cover pre-existing conditions, no matter what the condition is.
Call for FREE Help
(702) 898-0554
Health Insurance Quotes
Health Insurance Agent
Menu


Or… Just Call Us
(702) 898-0554
Fast and Easy – With Expert Help
One of our licensed agents will guide you step-by-step through your enrollment, answer your questions, and help you find the plan that’s right for you.
Begin Quote
click here
Continue Here
Finish Steps 3-4-5-6
You Have Already Completed
1). Calculate Your Income
This will determine your MAGI (Modified Adjusted Gross Income)
2). Determine Subsidy Eligibility
Using your MAGI, this chart will help determine if you qualify for a subsidy
On This Page
Begin comparing plans and selecting your coverage:
3). Location Options
Use the Nevada counties map to verify insurance availability
4). Select a Metal Tier
Choose between Platinum, Gold, Silver, or Bronze levels to balance your monthly premium with your potential out-of-pocket costs.
5). Compare Plan Networks & Coverage
Verify doctor and hospital networks, prescription coverage, and available urgent or emergency care.
6). Select Insurance Company & Plan
Compare available insurers and plans, reviewing premiums, deductibles, co-pays, coinsurance, and out-of-pocket maximums.
Step #3
Coverage by Location
Active Insurance Companies
Carrier Coverage by County
OFF Exchange
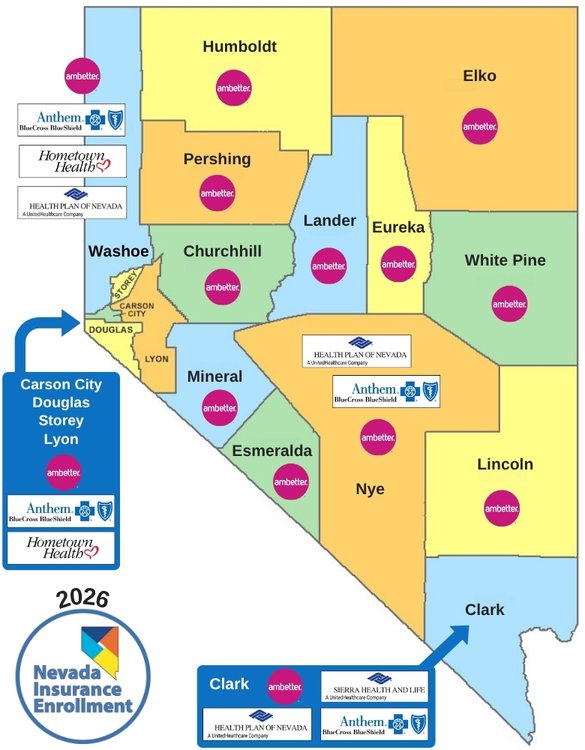

Health Plan of Nevada (HPN)
♦ HMO
♦ ON Exchange and OFF Exchange
>> ON Exchange: Serving ALL Nevada counties
>> OFF Exchange: Clark, Nye, Washoe
Sierra Health and Life
♦ EPO
♦ OFF Exchange only
♦ Clark County only
Ambetter from Silver Summit
♦ HMO
♦ Referrals to see a specialist are not required
♦ ON Exchange and OFF Exchange
♦ Serving ALL Nevada counties
Hometown Health
♦ Offering HMO & EPO in select counties
♦ OFF Exchange only
♦ Serving Carson City, Lyon, Washoe, Douglas, Storey
Anthem Blue Cross and Blue Shield
♦ HMO & EPO
♦ ON Exchange and OFF Exchange
♦ OFF Exchange – Carson City, Lyon, Washoe, Douglas, Storey, Nye, Clark
♦ ON Exchange – Serving ALL Nevada counties
♦ PPO only available for “Catastrophic” plans (under 30 years old)
Select Health
♦ HMO & EPO
♦ ON Exchange only
♦ Serving Nye and Clark County
Renown
♦ HMO
♦ ON Exchange only
♦ Serving Carson City, Washoe, Douglas, and Storey
Imperial Health
♦ HMO
♦ ON Exchange only
♦ Serving Washoe, Nye and Clark County
Molina Healthcare
♦ HMO
♦ ON Exchange only
♦ Serving Washoe, Nye and Clark County
CareSource
♦ HMO
♦ ON Exchange only
♦ Serving ALL Nevada counties
Step #4
Select a Metal Tier


PLATINUM | GOLD | SILVER | BRONZE
Platinum
covers90%of your medical bills until you reach your out-of-pocket maximum
Gold
covers80%of your medical bills until you reach your out-of-pocket maximum
Silver
covers70%of your medical bills until you reach your out-of-pocket maximum
Bronze
covers60%of your medical bills until you reach your out-of-pocket maximum
Step #5
Compare Plan Networks & Coverage


Focus on What Matters Most
When researching health insurance plans or speaking with your agent
Review Key Coverage Details
Then evaluate the options that best fit your needs
Start With the Essentials
-
Doctors & Clinics:
Check that your preferred providers are in-network
-
Prescriptions:
Verify your medications are covered
-
Hospitals & Urgent Care:
Make sure your nearby facilities are included
-
Plan Type:
Decide whether you want an HMO, PPO, or EPO
-
Travel Coverage:
See if you’re covered when traveling or relocating
-
Costs:
Compare deductibles, copays, and coinsurance
-
Out-of-Pocket Limit:
Note the maximum you might pay in a year
Then Consider Your Specific Needs
-
Chronic Conditions:
Coverage for ongoing care like diabetes, heart disease, or high blood pressure
-
Rehabilitation & Recovery:
Coverage for physical therapy, pain management, or post-surgery care
-
Behavioral Health Services:
Coverage for counseling, mental health, or substance abuse programs
-
Virtual Care Options:
Check if the plan includes telehealth or online visits, and whether your providers participate
-
Specialist Access:
Confirm that the types of specialists you may need (e.g., cardiologists, endocrinologists, orthopedists) are available in-network
Step #6
Select a Preferred Carrier


Health Insurance
From the Country's Top Insurance Companies
New for 2026
Battle Born State Plans are Affordable Care Act certified health plans designed to meet premium reduction targets.
(702) 898-0554
or
Begin Quote
click here
Let's Get You Enrolled
#1 - Call Us ⇒ to begin your enrollment / make appointment
OR
#2 - Fill out a short questionnaire ⇒ to request a quote / make appointment
Fast and Easy Enrollment
Enrolling into a health plan is fast and easy when you call one of our licensed and experienced health insurance agents.
Get Advice and Guidance
From a Licensed Local Health Insurance Agent
That Specializes in Nevada Health Plans




Please Be Careful…
So many times, we see honest, hard working people buying what they think are Qualified Health Insurance Plans...
only to find out later that their plan isn’t what they thought it was.
Then, when they find themselves in the hospital, they suffer the consequences of not understanding what they purchased and being severely underinsured.
Once you’ve terminated your qualified health insurance plan, if you don’t have a life event, you won’t be able to sign up for a new plan until the next Open Enrollment.
If the plan you are considering purchasing is a limited benefit medical plan, mini-medical plan, discount plan, indemnity plan, short-term plan, or looks and appears to be “insurance”, but does not cover the 10 “Essential Healthcare Benefits” then you are most likely buying a plan that is NOT considered to be a “Qualified Health Plan”. We STRONGLY recommend you do your research on these types of plans. Do a Google search or look at Yelp reviews of companies that sell these plans.
⇓
People are Selling FAKE Health Insurance
https://www.nevadainsuranceenrollment.com/health/insurance-scams/
Make Sure You're Buying a Qualified Health Plan


Qualified Health Plans are certified by Nevada Health Link verifying they provide the 10 essential health benefits. These plans follow required limits on how much you the member has to pay, and how much the insurance company pays. These health insurance plans meet rigorous requirements, including covering pre-existing conditions with no maximum lifetime or annual limits.
QHP’s (Qualified Health Plans):
Will Cover Your Medical Costs With NO Maximum Lifetime and Annual Limits
PLATINUM | GOLD | SILVER | BRONZE
♦ Platinum covers 90% of your medical bills until you reach your out-of-pocket maximum
♦ Gold covers 80% of your medical bills until you reach your out-of-pocket maximum
♦ Silver covers 70% of your medical bills until you reach your out-of-pocket maximum
♦ Bronze covers 60% of your medical bills until you reach your out-of-pocket maximum




Nevada's Premier Private Exchange
Where Nevadans Go To Enroll
Your Trusted Source for Private Health Plan Enrollment in Nevada
Proudly helping Nevadans find quality, affordable coverage for over 15 years


Nevada Health Link
Authorized Agent
Preffered Broker


National Association of Health Underwriters (NAHU)


Nevada Division of Insurance
Agent / Agency Search
Nevada Insurance Enrollment
National Producer License #17264164
Resident Producer Firm License #952196
Health Insurance is Confusing
Let Us Guide You
Don’t Live Nearby?
Kicking back on the patio? At the pool?
Still in your pajamas?



No Problem!
We Can Enroll You Remotely
We help clients all across Nevada. Whether you’re in Las Vegas, Reno, or anywhere in between.
You can enroll right from home! Call us, hop on a video chat, or join a secure screen-share session where you’ll see your agent’s screen as they walk you through every step of your enrollment.
Easy. Personal. Wherever you are.














