
Health Insurance in Las Vegas
Affordable Plans and Easy Enrollment Options
Purchase Health Insurance
From The Nation’s Top
Health Insurance Companies
Individual and Family Healthcare Across Nevada
♦ Free Help, Ongoing Support, Personalized Health Insurance Quotes
♦ Friendly, Local, Licensed Health Insurance Agents
♦ Trusted Healthcare Options for Nevadans
♦ Enrollment Made Easy
- In-Person
- Over the Phone
- Video Chat / screen-share


What is Health Insurance?
It’s Financial Protection
Because Accidents Happen
Health insurance is an agreement between you and the insurance company that helps cover the cost of medical care and protects you from overwhelming healthcare expenses. Instead of paying the entire bill yourself when you visit a doctor, fill a prescription, or go to the hospital, health insurance helps pay a portion of those costs.
Your health insurance plan also provides access to a network of doctors, specialists, hospitals, and pharmacies, along with preventive care, wellness programs, and cost-sharing features that help make your healthcare more affordable.
Many people refer to these health insurance policies as “Obamacare” insurance, major medical, or simply healthcare. These plans are Affordable Care Act (ACA) health insurance plans typically sold through the government’s federal marketplace (HealthCare.gov). In Nevada, however, enrollment is managed through the state’s exchange, called Nevada Health Link.
Menu
No Subsidy
Health Insurance
OFF Exchange
WITH Subsidy
Health Insurance
ON Exchange
Medicaid
Health Insurance
low income
NO Subsidy, WITH Subsidy, Medicaid [explanation] - click to open/close
1). WITH a Government Subsidy:
Where the Government helps you pay your premiums (You must qualify, based on your income and family size). If you want to apply for a Government subsidy you’ll be enrolling into a health insurance plan on the exchange, which is where you enroll.
2). With NO Government Subsidy:
You don’t qualify for a Government subsidy because you make too much money, OR you just don’t want a subsidy. No questions on income are required. If you want to buy your own plan without a Government subsidy, or know you won’t qualify for Government help because you make too much money each year, you can shop and enroll into health insurance “Off Exchange”, which means you are buying a health insurance plan in the private Market with no subsidy.
3). Medicaid:
Medicaid is a joint State/Federal health insurance program that is administered by the State. It provides health coverage for low-income individuals, especially pregnant women, children and the disabled. The Division of Welfare and Supportive Services (DWSS) determines eligibility for the Medicaid program.
Not Sure Which To Choose?
Start Here


⇒
Verify if you qualify for a health insurance subsidy, are eligible for Medicaid, or prefer a private health plan without a subsidy.
Check
Your
Eligibility
Use This Chart as a Quick Reference
If you fall within these limits, you’ll be able to calculate your exact subsidy amount on the next page.


2026 Health Insurance Subsidy Chart
by household size and income
The chart below lists the income numbers the IRS will use for subsidy eligibility.
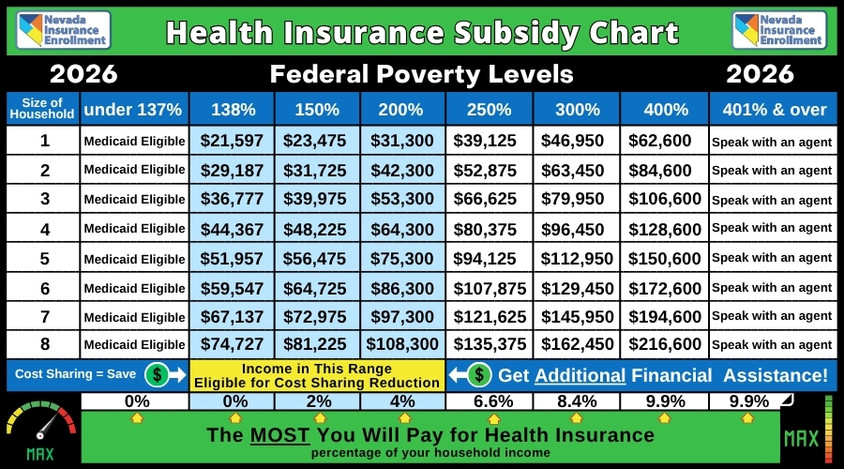

* The annual subsidy amounts change in January of each year
NOTE: You can buy a plan outside of the “Marketplace” that doesn’t have a subsidy
1). If your income is between 138% to 400%, you may be eligible for a health insurance subsidy.
2). If your income is between 138% to 200%, you may be eligible for a subsiby and additional benefits.
3). If your income is less than 138%, you may qualify for Medicaid. If it turns out you do not qualify for Medicaid after applying, come back to this page and begin enrollment.
Health Insurance Quotes
1). By Phone
(702) 898-0554
2). Online Quote
Short Questionnaire
3). In Person
4260 W. Craig Road #150-A
N. Las Vegas, NV 89032
Begin Quote
click here




Nevada’s Premier Private Exchange
Where Nevadans Go To Enroll
Why Work With Us?
We Are Professional Health Insurance Agents…
It’s What We Do
For over 15 years, Nevada Insurance Enrollment has specialized in health insurance.
- We are NOT seasonal staff
- We are NOT a faraway 1-800 number
- We ARE local, licensed agents
- We DO study Nevada plans
- We WILL guide you step-by-step
- We WILL help with billing, claims, membership
Why Do You Need Health Insurance?
Health insurance is a safeguard for both your health and your finances, providing financial protection and access to quality healthcare when you need it most. Whether it is managing a chronic condition, facing a sudden accident, unexpected illness, or requiring planned but costly surgeries, they can result in overwhelming medical expenses.
Note:
Not all health insurance plans cover the same services or pay the same amounts.
Choosing the right plan can make all the difference – for your healthcare and your budget.
Health Insurance Covers a Wide Range of Medical Needs
From Routine Care to Unexpected Emergencies
-
- Chronic Conditions: diabetes, asthma, high blood pressure
- Preventive: checkups, screenings, vaccines
- Accidents and Injuries: broken bones, sprains, cuts
- Surgeries: knee replacement, ACL repair, skin cancer
- Diagnostic and Labs: blood work, X-rays, MRIs, CT scans
- Mental Health Services: anxiety, depression
- Substance Abuse: drug or alcohol addiction
- Prescription Coverage: reduced cost of prescriptions
- Maternity: doctor visits, delivery, follow-up care
- Specialist Care: dermatologists, cardiologists, neurologists
- Family Support Services: marriage or family therapy
Even if you are healthy today, life can change in an instant. A car accident, a trip and fall, the arrival of a new baby, or a cancer diagnosis can happen without warning. In Las Vegas and across Southern Nevada, even a single ER visit or hospital stay can easily exceed thousands of dollars, sometimes reaching tens of thousands.
How Do You Get Health Insurance?
You Have Choices
The Difference Comes Down To:
-
- Local Guidance From Nevada Experts
- Support Beyond Open Enrollment
- Service Tailored to Your Needs
(702) 898-0554
or
Begin Quote
click here
Unlike group health insurance you receive from your employer or spouse’s employer, individual and family health insurance plans you purchase on your own. When you buy health insurance on your own, it is a private health insurance plan and gives you the flexibility to choose a plan that fits your needs and budget.
Enrollment Made Simple
Purchasing health insurance may feel overwhelming, but it does not have to be complicated. You have several options for enrollment, whether through the state’s Marketplace (Nevada Health Link), directly with an insurance company, an online broker, or with the help of a licensed local health insurance agent.
Same Price
The important thing to know is that no matter which path you choose, the price of your health plan will always be the same. Whether you choose to purchase on your own, online, or with the help of a licensed agent, your premium does not change. The agents services are always free.
The real difference lies in the level of guidance and support you receive.
Enrollment Options:
Which One Is Right for You?


Local Agents
Your Free Resource
When it comes to choosing health insurance, nothing compares to the support of a local licensed health insurance agent. Our agents study every plan from every carrier available in Nevada, comparing cost, coverage, and benefits.
Why Work With Us?
For over 15 years, Nevada Insurance Enrollment has specialized in health insurance. We are not seasonal staff or a faraway 1-800 number. We are local, licensed agents who study Nevada plans, guide you step-by-step, and stay with you for billing, claims, or membership questions long after enrollment. If you ever have questions, you will speak to your agent, the same person who already knows you and your situation.
We are professional health insurance agents… it’s what we do.
The important thing to know is that no matter which path you choose, the price of your health plan will always be the same. Whether you choose to purchase on your own, online, or with the help of a licensed agent, your premium does not change. The agents services are always free.
The real difference lies in the level of guidance and support you receive.
(702) 898-0554


Do It Yourself
You can enroll through Nevada Health Link or work directly with a health insurance company. This may work if you already know exactly what you want, but there is no personal guidance if you are unsure about networks, doctors, prescriptions, subsidy eligibility, co-pays, deductibles, or other benefits.
If you need help later, whether it is a billing question, prescriptions, making changes, requesting authorization, or filing a claim, you will need to call the insurance company’s customer service line yourself.
Did You Know?
Keep in Mind:
Licensed local health insurance agents (like us) are different. We can manage everything for you – questions, communication, changes, authorizations, and claims.
Plus, our help is always free. Your premium does not change. Enrolling on your own does not save money, it only means you will not have an expert to guide you if questions or problems come up later.


Use a 'Navigator'
Navigators are certified enrollment counselors trained by Nevada Health Link. To qualify, they must complete a 20-hour training course, pass an exam, and clear a background check. Navigators provide free assistance with applications, documents, and general education about Marketplace rules.
Did You Know?
Worth Noting:
While the 20-hour training course for a Navigator may provide a basic foundation, it is not the same as the licensing, ongoing training, and years of direct experience that professional health insurance agents offer.


Online Brokers
Online Brokers (like e-Health and HealthSherpa) operate privately owned websites that let you browse and compare plans from multiple insurers at your own convenience, anytime. While these platforms can be convenient and may look easy to use, their services come with important limitations.
These websites serve customers nationwide, not just Nevada. They do not specialize in Nevada health insurance plans or understand the nuances of Nevada Health Link, local doctor and hospital networks, or state-specific rules.
If you have questions, or need help in the future, you will call a 1-800 number and speak with a random representative.
Did You Know?
The Reality Is:
The price of your health insurance policy will always be the same, no matter where you buy it. Choosing to purchase your health insurance through an online broker does not save you money, it only means you lose out on personalized local guidance and ongoing support from a local, licensed health insurance agent.
Health Insurance Open Enrollment Has Ended
You Can Only Buy Health Insurance During This Time
November 1st, 2025 ⇒ January 15th, 2026
unless you have a ‘Life Event’
After 1/15/2026
You Will Need a Life Event To Get Health Insurance
Open Enrollment
Extended Hours
Begin Quote
click here


Or… Just Call Us
(702) 898-0554
Fast and Easy – With Expert Help
One of our licensed agents will guide you step-by-step through your enrollment, answer your questions, and help you find the plan that’s right for you.
2026 Health Insurance
Follow These Six Steps
You’ll Begin Working Through These Steps On The Next Page
1). Calculate Your Income
This will determine your MAGI (Modified Adjusted Gross Income)
2). Determine Subsidy Eligibility
Use your MAGI to see if you qualify for a subsidy.
3). Location Options
Use the Nevada counties map to verify insurance availability
4). Select a Metal Tier
Choose between Platinum, Gold, Silver, or Bronze levels to balance your monthly premium with your potential out-of-pocket costs.
5). Compare Plan Networks & Coverage
Verify doctor and hospital networks, prescription coverage, and available urgent or emergency care.
6). Select Insurance Company & Plan
Compare available insurers and plans, reviewing premiums, deductibles, co-pays, coinsurance, and out-of-pocket maximums.
Begin Quote
click here
Health Insurance Quotes
1). By Phone
(702) 898-0554
2). Online
Short Questionnaire
3). In Person
4260 W. Craig Road #150-A
N. Las Vegas, NV 89032
(702) 898-0554


Let’s Get You Enrolled
choose an option
-
Call Us ⇒ to begin your enrollment / make appointment
-
Fill out a short questionnaire ⇒ to request a quote / make appointment
-
Select an option below ⇒ to continue your research / enrollment
Begin Quote
click here
Still Not Sure?
Start Here
We’ll help you find out if you qualify for a health insurance subsidy, are eligible for Medicaid, or prefer a private health plan without a subsidy.
Check
Your
Eligibility
No Subsidy
Health Insurance
OFF Exchange
WITH Subsidy
Health Insurance
ON Exchange
Medicaid
Health Insurance
low income
What is Health Insurance?
-
What is Health Insurance?
It’s Financial Protection - Because Accidents Happen Health insurance is an agreement between you and the insurance company that helps cover the cost of medical care and protects you from overwhelming healthcare expenses. Instead of paying the entire bill yourself when you visit a doctor, fill a prescription, or go to the hospital, health insurance helps pay a portion of those costs. Your health insurance plan also provides access to a network of doctors, specialists, hospitals, and pharmacies, along with preventive care, wellness programs, and cost-sharing features that help make your healthcare more affordable. Many people refer to these health insurance policies as “Obamacare” insurance, major medical, or simply healthcare. These plans are Affordable Care Act (ACA) health insurance plans typically sold through the government’s federal marketplace (HealthCare.gov). In Nevada, however, enrollment is managed through the state’s exchange, called Nevada Health Link. Read More: https://www.nevadainsuranceenrollment.com/health-insurance/ -
Why Do You Need Health Insurance?
Health insurance is a safeguard for both your health and your finances, providing financial protection and access to quality healthcare when you need it most. Whether it is managing a chronic condition, facing a sudden accident, unexpected illness, or requiring planned but costly surgeries, they can result in overwhelming medical expenses. Read More: https://www.nevadainsuranceenrollment.com/health-insurance/ -
What Does Health Insurance Pay For?
Health Insurance Covers a Wide Range of Medical Needs From Routine Care to Unexpected Emergencies- Chronic Conditions: diabetes, asthma, high blood pressure
- Preventive: checkups, screenings, vaccines
- Accidents and Injuries: broken bones, sprains, cuts
- Surgeries: knee replacement, ACL repair, skin cancer
- Diagnostic and Labs: blood work, X-rays, MRIs, CT scans
- Mental Health Services: anxiety, depression
- Substance Abuse: drug or alcohol addiction
- Prescription Coverage: reduced cost of prescriptions
- Maternity: doctor visits, delivery, follow-up care
- Specialist Care: dermatologists, cardiologists, neurologists
- Family Support Services: marriage or family therapy
-
Where Should I Buy My Health Insurance?
You Have Choices. The Difference Comes Down To:1. Local Guidance From Nevada Experts 2. Support Beyond Open Enrollment 3. Service Tailored to Your Needs
Unlike group health insurance you receive from your employer or spouse’s employer, individual and family health insurance plans you purchase on your own. When you buy health insurance on your own, it is a private health insurance plan and gives you the flexibility to choose a plan that fits your needs and budget. Enrollment Made Simple Purchasing health insurance may feel overwhelming, but it does not have to be complicated. You have several options for enrollment, whether through the state’s Marketplace (Nevada Health Link), directly with an insurance company, an online broker, or with the help of a licensed local health insurance agent. Same Price The important thing to know is that no matter which path you choose, the price of your health plan will always be the same. Whether you choose to purchase on your own, online, or with the help of a licensed agent, your premium does not change. The agents services are always free. The real difference lies in the level of guidance and support you receive. Enrollment Options: Which One Is Right for You? Local Agents Your Free Resource When it comes to choosing health insurance, nothing compares to the support of a local licensed health insurance agent. Our agents study every plan from every carrier available in Nevada, comparing cost, coverage, and benefits. Why Work With Us? For over 15 years, Nevada Insurance Enrollment has specialized in health insurance. We are not seasonal staff or a faraway 1-800 number. We are local, licensed agents who study Nevada plans, guide you step-by-step, and stay with you for billing, claims, or membership questions long after enrollment. If you ever have questions, you will speak to your agent, the same person who already knows you and your situation. We are professional health insurance agents… it’s what we do. The important thing to know is that no matter which path you choose, the price of your health plan will always be the same. Whether you choose to purchase on your own, online, or with the help of a licensed agent, your premium does not change. The agents services are always free.
Do It Yourself You can enroll through Nevada Health Link or work directly with a health insurance company. This may work if you already know exactly what you want, but there is no personal guidance if you are unsure about networks, doctors, prescriptions, subsidy eligibility, co-pays, deductibles, or other benefits. If you need help later, whether it is a billing question, prescriptions, making changes, requesting authorization, or filing a claim, you will need to call the insurance company’s customer service line yourself. Keep in Mind: Licensed local health insurance agents (like us) are different. We can manage everything for you – questions, communication, changes, authorizations, and claims. Plus, our help is always free. Your premium does not change. Enrolling on your own does not save money, it only means you will not have an expert to guide you if questions or problems come up later.
Use a 'Navigator' Navigators are certified enrollment counselors trained by Nevada Health Link. To qualify, they must complete a 20-hour training course, pass an exam, and clear a background check. Navigators provide free assistance with applications, documents, and general education about Marketplace rules. Worth Noting: While the 20-hour training course for a Navigator may provide a basic foundation, it is not the same as the licensing, ongoing training, and years of direct experience that professional health insurance agents offer.
Online Brokers Online Brokers (like e-Health and HealthSherpa) operate privately owned websites that let you browse and compare plans from multiple insurers at your own convenience, anytime. While these platforms can be convenient and may look easy to use, their services come with important limitations. These websites serve customers nationwide, not just Nevada. They do not specialize in Nevada health insurance plans or understand the nuances of Nevada Health Link, local doctor and hospital networks, or state-specific rules. If you have questions, or need help in the future, you will call a 1-800 number and speak with a random representative. The Reality Is: The price of your health insurance policy will always be the same, no matter where you buy it. Choosing to purchase your health insurance through an online broker does not save you money, it only means you lose out on personalized local guidance and ongoing support from a local, licensed health insurance agent. Read More: https://www.nevadainsuranceenrollment.com/insurance-agent/ -
Will My Health Insurance Cost More If I Use an Agent?
NO. We know people on social media say it will, and that using an agent will cost you more because they get paid a commission, but that is misinformation. The truth is, having an agent help and guide you doesn’t cost anything (the service we offer is FREE). The INSURANCE COMPANY pays the agent to assist you, and you will NOT pay a higher rate because of our help. It's All The Same Price The important thing to know is that no matter which path you choose, the price of your health plan will always be the same. Whether you choose to purchase on your own, online, or with the help of a licensed agent, your premium does not change. The agents services are always free. Choosing to purchase your health insurance without professional guidance doesn't save you money, it only means you lose out on personalized local guidance and ongoing support from a local, licensed health insurance agent. The real difference lies in the level of guidance and support you receive. Why Use a Health Insurance Agent? Professional health insurance agents help and guide you. With their knowledge and expertise, they take you step-by-step through the plans (from the available health insurance companies) and find the best plan for the best price. Local Agents Your Free Resource When it comes to choosing health insurance, nothing compares to the support of a local licensed health insurance agent. Our agents study every plan from every carrier available in Nevada, comparing cost, coverage, and benefits. We live in Las Vegas, and can manage everything for you – questions, communication, changes, authorizations, and claims. Why Work With Us? We are professional health insurance agents… it’s what we do. For over 15 years, Nevada Insurance Enrollment has specialized in health insurance. We are not seasonal staff or a faraway 1-800 number. We are local, licensed agents who study Nevada plans, guide you step-by-step, and stay with you for billing, claims, or membership questions long after enrollment. If you ever have questions, you will speak to your agent, the same person who already knows you and your situation.





